Vegetative chronic genital herpes is an atypical presentation of herpes simplex 2 that it is usually seen in patients coinfected with human immunodeficiency virus. Clinically, it is characterized by extensive ulcers that evolve to chronification and hypertrophic pseudotumor forms. Antiviral drugs are recommended for the treatment, and acyclovir is the most used one. Foscarnet is the treatment of choice to resistant cases, although treatment failure has been reported. We report a male patient, previously diagnosed with human immunodeficiency virus who developed vegetative chronic genital herpes resistant to acyclovir and successfully treated with imiquimod.
Genital herpes is one of the most prevalent sexually transmitted diseases in the world. It is caused by the herpes simplex virus (HSV). The disease can be asymptomatic or present itself with different clinical features. HSV-2 is the most common serotype associated to genital herpes. Clinically, it can vary from erosive balanitis to vulvitis or painful vaginitis.1
A large number of recurrences and atypical presentations of HSV skin lesions have been reported in individuals coinfected with human immunodeficiency virus (HIV). In contrast, HSV infection increases the risk of HIV transmission and disease progression. Genital herpes ulcers can be larger in these patients and, in rare cases, it can become hypertrophic and vegetative.2
Vegetative chronic genital herpes is difficult to treat. Some reports reveal no response or several recurrence cases after treatment with antiviral drugs.2 We report a case of a male patient infected with HIV presented with vegetative chronic genital herpes successfully treated with imiquimod.
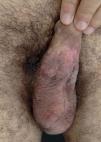
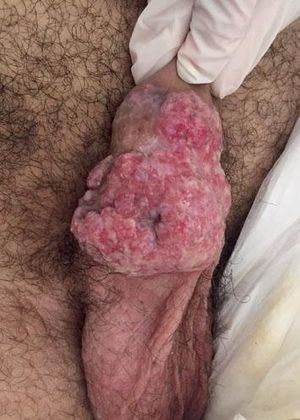
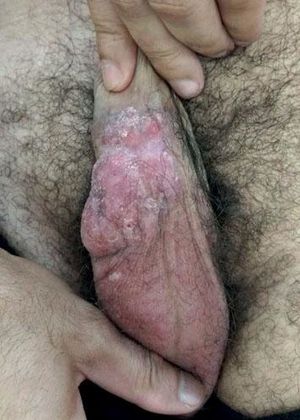
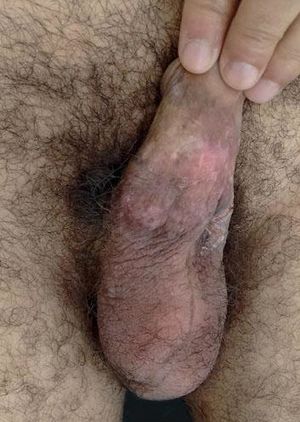
Case ReportA 41-year-old Caucasian male patient diagnosed with acquired immunodeficiency syndrome three years ago, using Lopinavir/Ritonavir and maintaining an undetectable viral load presented with ulcerative and vegetative skin lesion on the body of the penis for five months. The lesion started small and grew progressively (Figure 1). A skin biopsy was performed three months before, and histopathological examination suggested chronic herpes. The patient was treated with oral acyclovir for 7 days. Due to the lack of response, he was hospitalized and was started on IV acyclovir, but also showed no response after 14 days. A new biopsy was performed and immunohistochemical study was positive for HSV-1 and HSV-2, confirming the diagnosis of conic herpes. We opted for topical treatment with imiquimod 5% cream 3 times a week during 2 weeks. Because of the patient’s good tolerance and favorable response to the drug (Figure 2), we increased dosage to 5 times a week for 4 more weeks and application under occlusion. After 12 weeks of treatment, we observed an excellent response with total healing of the lesion (Figure 3).
DiscussionVegetative chronic genital herpes is a dramatic clinical presentation that may arise mainly in patients that are also infected with HIV. It is characterized by painful, vegetative, and exudative ulcers.2 Biopsy is important to exclude neoplastic and other infectious diseases. Although systemic antiviral drugs don’t seem to be effective, foscarnet has a variable efficacy, resulting in many episodes of recurrence.2,3
Imiquimod is an immune response modulator with an indirect antiviral and antitumoral responses.2,4 The exact mechanism by which it acts as an antiviral is still unknown. It induces the endogenous synthesis of many cytokines, as interferon alpha (IFN-α), tumor necrosis factor (TNF), and interleukins, which are involved in T helper type 1 (TH1) response activation. It results in the production of interferon gama, a powerful antiviral cytokine.5
This topical medicine is approved for treatment of external genital warts, caused by human papilloma virus (HPV).5 The efficiency of imiquimod 5% cream is not well established in the literature, but its use has been described to treat some cases of hypertrophic genital lesions.2
In 2006, Brummitt reported the case of a patient with an exophytic perianal lesion resistant to acyclovir, ganciclovir, valaciclovir. Also, the lesion recurred after treatment with foscarnet. After treatment with imiquimod 5% cream for 12 weeks 3 times a week, the patient had a good response.3 In 2007, Abbo and Vincek reported the case of a patient with severe immunosuppression who presented with vegetative herpes on the penis and scrotum. The lesion was successfully treated with imiquimod 3 times a week associated with famciclovir. The treatment resulted in total remission of the skin lesions after 2-8 weeks of treatment.6
Lestre and João also described the posology of 3 times a week during the first 2 weeks, then 5 times a week for 8 more weeks. This increase in famciclovir dosage can lead to a faster response, without causing any more side effects.2 The authors also consider that application under occlusion can potentialize treatment efficacy, which inspired the prescribed treatment for our patient.
Vegetative genital chronic herpes has been seen in literature as difficult to manage, with many reports of resistance or recurrence after treatment with the available systemic antiviral drugs. We report the case of a satisfactory response after the use of imiquimod cream, in agreement with positive experiences previously described in literature. We understand that performing comparative and random allocation studies would be important to define treatment protocols for this disease presentation.